Our History and Milestones in the Research and Treatment of Cancer and Blood Disorders
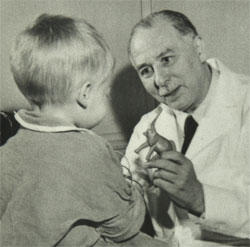
More than 70 years ago, Dr. Sidney Farber refused to accept that childhood cancer was untreatable, and his determination led to the development of chemotherapy and the first remissions of childhood leukemia.
Today, we continue Dr. Farber’s legacy through research that has yielded many of the advances in care used today. Here are some highlights of our team’s long history of accomplishments:
- 1932 – At Boston Children’s Hospital, Dr. Louis Diamond – often said to be the “father of pediatric hematology” – characterizes Rh disease, in which a fetus's blood is incompatible with its mother's. Dr. Diamond later develops exchange transfusion to treat the disease.
- 1938 – At Boston Children’s Hospital, Dr. Louis Diamond and Dr. Kenneth Blackfan are the first to describe Diamond-Blackfan anemia, a rare blood disorder.
- 1946 – A specialized hematology/oncology program at Boston Children's Hospital is formed. It is co-led by Dr. Louis Diamond and Dr. Sidney Farber.
- 1947 – Dr. Sidney Farber and his team of clinicians and laboratory scientists are the first to use chemotherapy to treat cancer; they achieve the world’s first successful remission of acute lymphoblastic leukemia.
- 1947 – Dr. Sidney Farber founds the Children's Cancer Research Foundation (which later becomes Dana-Farber Cancer Institute), and he develops the first research program in chemotherapy for children with cancer. Dr. Farber’s program is the first-ever cancer program for children to provide “total care” – clinical care, nutrition, social work, counseling, and more – in one place. Today, this model is the standard for pediatric and adult cancer centers.
- 1951 – The Jimmy Fund Building to treat childhood cancer patients is completed, located adjacent to Boston Children's Hospital. Childhood cancer patients receive outpatient care in the Jimmy Fund Building, while surgery and inpatient care continue to be provided at Boston Children's Hospital.
- 1955 – Dr. Sidney Farber and colleagues achieve the first remissions in Wilms tumor of the kidney, a common form of childhood cancer. By employing the antibiotic actinomycin D in addition to surgery and radiation therapy, they boost cure rates from 40 to 85 percent.
- 1964 – Drs. Harry Shwachman and Louis Diamond are the first to describe Shwachman-Diamond syndrome, a rare, inherited blood disorder.
- 1967 – Dr. David Nathan becomes Division Chief of the Hematology/Oncology Program at Boston Children’s.
- 1968 – Drs. David Nathan and Harold Zarkowsky describe the pathophysiology of hereditary stomatocytosis.
- 1968 – Drs. Robert Baehner and David Nathan describe the NBT test for chronic granulomatous disease, a diagnostic test that also helped pinpoint the key underlying molecular defect in the disease.
- 1972 – Drs. YW Kan, Blanche Alter, and David Nathan describe the first intrauterine diagnosis of sickle cell anemia.
- 1972 – Dr. Thomas Stossel publishes the first of many years of seminal studies that define the mechanism of phagocytosis.
- 1973 – The Children's Cancer Research Foundation receives federal designation as a regional comprehensive cancer center. Dr. Sidney Farber passes away.
- 1973 – Drs. Emil Frei lll and Stephen Sallan start the first in an ongoing series of clinical trials for children diagnosed with acute lymphoblastic leukemia (ALL). These clinical trials, now provided through the DFCI/ALL Consortium, dramatically improve treatment and play a key role in building toward today’s cure rates of 85-90%.
- 1973 – Drs. Ronald McCaffrey and David Baltimore identify terminal deoxynucleotidyl transferase as a marker for acute lymphoblastic leukemia.
- 1974 – The Children's Cancer Research Foundation is renamed the Sidney Farber Cancer Center in recognition of its founder. Dr. Emil Frei III becomes the new Center director.
- 1974 – Drs. David Nathan and Bertil Glader describe hereditary xerocytosis.
- 1974 – Drs. Bernard Forget and Edward Benz discover that messenger RNA for beta globin is absent in patients with beta(0) thalassemia.
- 1975 – Drs. John Hartwig and Thomas Stossel discover actin binding protein, a key protein responsible for the branching of actin filaments in all cells.
- 1976 – Drs. David Nathan and Blanche Alter develop an in-utero diagnostic test for thalassemia, a serious inherited blood disorder.
- 1976 – Drs. David Nathan, Susan Shurin, and Richard Propper develop parenteral desferrioxamine as a therapy for iron overload (toxicity) in thalassemia and related blood conditions.
- 1977 – Drs. Emil Frei lll and Norman Jaffe use pre-operative chemotherapy to facilitate the world's first limb-salvage surgeries by Dr. Hugh Watts for children with osteosarcoma. This leads to increased cure rates and improved quality of life.
- 1978 – Dr. Stuart Orkin develops restriction endonuclease mapping (genetic tests) to diagnose thalassemia in unborn children. A similar technique leads to the development of prenatal tests for sickle cell anemia in 1982.
- 1982 – Drs. Lawrence Wolfe and Samuel Lux discover the first functional molecular defect in hereditary spherocytosis.
- 1983 – The Sidney Farber Cancer Institute is renamed Dana-Farber Cancer Institute in honor of the financial support from the Charles A. Dana Foundation.
- 1984 – Drs. Orah Platt and David Nathan discover that hydroxyurea raises fetal hemoglobin. Hydroxyurea quickly becomes – and currently still is – the best therapy for sickle cell anemia.
- 1984 – Dr. Orah Platt publishes the first of a series of landmark studies on growth and development, pain crises, and mortality in sickle cell anemia.
- 1984 – Dr. David Williams develops retroviral vectors for the introduction of genes into hematopoietic stem cells, the technique that lays the ground work for gene therapy.
- 1985 – Dr. David Nathan becomes Chair of Pediatrics and Physician-in-Chief at Boston Children's Hospital. Dr. Samuel Lux becomes Division Chief of Hematology/Oncology at Boston Children's Hospital. Steven Burakoff becomes Department Chair of Pediatric Oncology at Dana-Farber Cancer Institute.
- 1986 – Dr. Stuart Orkin and his research team develop the technique of positional cloning to identify the genes responsible for chronic granulomatous disease.
- 1986 – Stephen Friend discovers and clones the recessive oncogene, Rb.
- 1986 – Drs. David Ginsburg and Stuart Orkin define the structure of von Willebrand factor, a key to understanding the important coagulation disorder that results from absence or malfunction of the factor.
- 1987 – Dr. Steven Burakoff shows that CD4, the HIV receptor and a key molecule on helper T cells, is critical for enhancing T cell responsiveness when suboptimal amounts of antigen are present.
- 1988 – Two out of every three children who enter the Jimmy Fund Clinic are cured.
- 1988 – Drs. Alan Ezekowitz, Mary Dinauer, Stuart Orkin, and Peter Newburger show that gamma interferon is an effective therapy in chronic granulomatous disease.
- 1989 – Dr. Alan D’Andrea clones the erythropoietin receptor, which controls red blood cell production.
- 1993 – A team at Boston Children’s Hospital led by Dr. Carlo Brugnara discovers that a common antifungal medication, clotrimazole, prevents dehydration in red blood cells, a factor in sickle cell disease.
- 1993 – Dr. Lisa Diller is the founding director of the David B. Perini Jr. Quality of Life Clinic, one of the nation’s first programs for survivors of childhood cancer.
- 1997 – Drs. Cameron Trenor, Mark Fleming, and Nancy Andrews discover and clone the first iron transporter.
- 1997 – Dr. Joanne Wolfe founds the Pediatric Advanced Care Team (PACT), a groundbreaking model pediatric palliative care program. Dr. Wolfe is widely recognized as a pioneer in pediatric palliative care.
- 1998 – Dr. David Fisher describes the genetic pathway of melanocyte differentiators.
- 1998 – Dr. Leonard Zon publishes the first in a series of pioneering studies that establish zebrafish genetics as a key tool in understanding hematopoietic and vascular development.
- 1999 – Dr. Todd Golub first uses gene expression microarrays to differentiate cancers.
- 2000 – Dana-Farber/Children’s Hospital Cancer Center (later renamed Dana-Farber/Boston Children’s Cancer and Blood Disorders Center) is created, formalizing the 50-year-plus relationship between Dana-Farber and Boston Children’s Hospital.
- 2000 – Dr. Stuart Orkin becomes Department Chair of Pediatric Oncology at Dana-Farber Cancer Institute.
- 2000 – A study by Stephan Grupp, Lisa Diller, and colleagues finds that induction chemotherapy followed by tandem high-dose therapy and peripheral blood stem-cell rescue in rapid sequence significantly improve survival rates for children with high-risk neuroblastoma.
- 1994-2001 – Dr. Alan D’Andrea describes many of the genes in the Fanconi anemia pathway, including how they function and interact with each other and with other DNA repair pathways.
- 2001 – Dr. Alan D’Andrea discovers that genes linked to Fanconi anemia are also involved in switching on BRCA1, a gene that, when defective, is the most common source of inherited breast cancer.
- 2001 – The Center for Experimental Medicine at Dana-Farber is established in efforts to convert laboratory advances into better treatments for patients.
- 2003 – A study by Dr. Holcombe Grier finds that the addition of ifosfamide and etoposide to standard chemotherapy greatly improves survival rates in patients with Ewing's sarcoma or primitive neuroectodermal tumor of bone.
- 2004 – Dr. Loren Walensky creates stapled peptides, which are used for peptidomimetic therapeutics.
- 2006 – Dr. Scott Armstrong and colleagues identify self-renewal genes that turn a normal blood cell progenitor into a leukemic stem cell. The cells have proven surprisingly different from normal blood stem cells, potentially making it possible to selectively target them with drugs.
- 2006 – Dr. David Pellman discovers a set of genes whose loss is only lethal in hyperdiploid cells and are therefore therapeutic targets in hyperdiploid cancer cells.
- 2007 – Dr. Len Zon discovers that prostaglandin E2 greatly stimulates the growth of blood and probably other tissue stem cells.
- 2007 – Dr. Stuart Orkin and colleagues show that difficult-to-treat myeloproliferative syndromes, which can progress to leukemia, are rooted not in errant blood stem cells, as previously thought, but in the cells' surrounding environment. The new understanding helps explain why normal blood stem cells transplanted into patients with myeloproliferative syndromes sometimes become diseased themselves, and may pave the way to novel therapies.
- 2007 – Dr. David Williams becomes Division Chief of Hematology/Oncology at Boston Children's Hospital.
- 2008 – A study led by Dr. Scott Armstrong discovers a small but potent epigenetic change (a change in gene activation) that launches a hard-to-treat form of acute lymphoblastic leukemia. As a result of a mutation, an enzyme called DOT1L abnormally alters chromosome structure and activates genes that are normally silent.
- 2008 – Drs. Vijay Sankaran and Stuart Orkin discover that the fetal hemoglobin to adult hemoglobin switch is controlled by the BCL11A transcription factor. This factor can reawaken red blood cells' ability to produce a fetal form of hemoglobin (HbF) that can compensate for the lack of functional adult hemoglobin. This solves a decades-old problem in hematology and has important implications for the treatment of sickle cell disease and thalassemias.
- 2008 – Dr. George Daley discovers how to reprogram human somatic cells to pluripotent stem cells with defined transcription factors.
- 2008 – Dr. Rani George finds that activating mutations in the receptor tyrosine kinase ALK cause some cases of neuroblastoma.
- 2009 – Drs. George Daley and Richard Gregory show that the microRNA, Lin 28, plays an important role in germ cell development and cancer.
- 2009 – Drs. Len Zon and George Daley discover that blood flow triggers development of hematopoietic stem cells.
- 2011 – Drs. Luigi Notarangelo, Sung-Yun Pai, and David Williams achieve the first successful treatment of severe combined immunodeficiency, commonly known as “Bubble Boy” Syndrome, by gene therapy in the US.
- 2011 – Drs. Vijay Sankaran and Stuart Orkin successfully correct sickle cell disease in mice by turning off a single gene and restoring red blood cells' ability to produce a fetal form of hemoglobin. This approach may be the key to treating other anemias and other blood disorders such as beta thalassemia.
- 2014 – A study by Dr. Peter Manley finds that children with low-grade gliomas have increased long-term survival if they do not receive radiation therapy.
- 2014 – Although women who survive childhood cancer face an increased risk of infertility, Dr. Lisa Diller finds that nearly two-thirds of those who tried unsuccessfully to become pregnant for at least a year eventually conceived – comparable to the rate of eventual pregnancy for all clinically infertile women.
- 2015 – A study by Dr. Vijay Sankaran finds that turning off the SH2B3 gene increases the production of red blood cells from stem cells roughly 300-500%. These findings suggest a way to cost-effectively manufacture red blood cells from stem cells, which could help children with rare blood disorders.
- 2015 – A study by Dr. Lewis Silverman finds that prophylactic antibiotics significantly reduce the risk of serious bacterial infections in children during the critical first month of treatment for acute lymphoblastic leukemia (ALL). While the overall cure rate for ALL is high, about one to two percent of children with ALL die during the first month of therapy from treatment complications, primarily infection-related.
- 2016 – A study led by Dr. Katherine Janeway finds that clinical genomic sequencing is feasible in pediatric oncology and can be used to recommend therapy or pinpoint diagnosis in children with solid tumors.
- 2016 – In a study by Dr. David A. Williams, Christian Brendel, PhD, and Swaroopa Guda, PhD, BCL11A-based gene therapy for sickle cell disease passes a key preclinical test. The work sets the stage for bringing a recent discovery in Dr. Stuart Orkin’s laboratory about fetal hemoglobin to a curative gene therapy treatment of sickle cell disease.
- 2016 – A study by Dr. Lisa Diller finds that children with high-risk neuroblastoma whose treatment included two autologous stem-cell transplants were more likely to be free of cancer three years later than patients who underwent a single transplant.
- 2017 – A study by Dr. Vijay Sankaran finds a mutation in the erythropoietin gene causes a change in binding to the erythropoietin receptor. Through this research, an easily treatable new type of transfusion-dependent anemia similar to Diamond-Blackfan anemia is defined.

 Translate
Translate